Light Propagation in Tissue
Introduction:
Biological tissue is typically treated as an absorbing and scattering medium and various methods have been developed to understand the optical and thermal responses of tissue due to its interaction with light. In this module, the optical processes involved in light tissue interaction will be described. In general, the way light will interact with tissue is a complicated interplay of tissue properties and light (laser) properties. Since the optical and thermal responses of tissue due to light are highly dependent on the characteristics of the laser source, a description of the various laser parameters and their influence upon tissue response is given first. Basic irradiation parameters for establishing dosimetry requirements for any laser therapeutic procedure are:
1) power, irradiation time, and spotsize for continuous wave (cw) lasers, and
2) energy per pulse, irradiation time, spotsize, repetition rate, and number of pulses for pulse lasers.
Perhaps the most important cw irradiation parameter is irradiance (W/m2). The irradiance is a function of the power delivered and the spotsize on the tissue. Low irradiances that do not significantly increase tissue temperature are associated with diagnostic applications, photochemical processes, and biostimulation, while high irradiances can ablate tissue and create mechanical damage in the tissue. The depth at which laser light effects tissue depends upon the optical properties of tissue which vary with wavelength. The optical properties and the role they play in determining how light is distributed in tissue, are the main topics of this module.
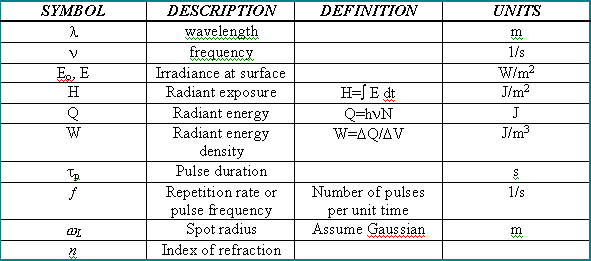
The basic irradiation parameters are
RADIANT POWER- the power of a source (also known as flux) is described by its radiant power (P). If one could enclose a source within a box and capture all the energy radiating from the source, the energy per unit time, J/sec, in the box would equal the radiant power (watts).
RADIANT ENERGY- a source with a power output (P in watts) that is turned on for a time (t in seconds) will yield a radiant energy (Q in joules)
Q = P* t
IRRADIANCE (E in W/m2) - at a point on a surface, is the radiant power incident on an element of the surface divided by the area of the surface
E = P/A
RADIANT EXPOSURE (H0 in J/m2)- (used for pulsed energy sources) - at a point of a surface, is the radiant energy incident on an element of the surface divided by the area of the surface
H = Q/A
The propagation of photons (light) within tissue is governed by several equally probable events, which include absorption and scattering within the tissue as well as reflection and transmission at the boundaries of the tissue. An exact assessment of light propagation in tissue would require a model that characterized detailed spatial distribution of tissue structures along with their sizes, their absorbing properties and their refractive indices. However, for real tissue (e.g. skin), such a task of creating a precise representation with as a computer simulation or a tissue phantom is not quite feasible. Thus for the purpose of understanding light propagation in tissue in a reasonable sense, tissue is treated as an absorbing material with scatterers randomly distributed over the volume. The material is assumed to be isotropic and homogeneous.
References:
1. Welch & Van Gemert, 1989, Clinical Use of Laser-Tissue Interactions. IEEE
2. Welch & Van Gemert, 1995, Optical Thermal Response of Laser-Irradiated Tissue, Plenum Press
Tissue Optics
The two fundamental tasks of the field of tissue optics are:
1) Find the light per unit area per unit time that reaches a target chromophore at some position, r, in the tissue and determine how much of that light is absorbed.
2) Determine the absorption and scattering properties of tissue.
In describing the optical properties and light propagation in tissues, light is treated as photons. Photons in a turbid medium such as tissue can move randomly in all directions and may be scattered (described by its scattering coefficient µs [m-1]) or absorbed (described by its absorption coefficient µa [m-1]). These coefficients along with anisotropy (i.e. the direction in which a photon is scattered if it is scattered) and index of refraction are referred to as the optical properties of a material.
First let's consider a slab of tissue. If photons are hitting the tissue several things can happen:

1) Some photons will reflect off the surface of the material (similar to what happens to glass and other materials - Fresnel's equations hold for tissue as well)
2) The majority of the photons will enter the tissue upon which the following can happen:
a) the photon is absorbed (and can be converted to heat, trigger a chemical reaction or cause fluorescence emission)
b) the photon is scattered (bumps into a particle and changes direction but continues to exist)
c) nothing (some photons can make it through the entire slab without running into anything, they are neither scattered nor absorbed and will emerge on the other side - these are called ballistic photons).
For now let's forget about scattering and consider absorption first.
Absorption
In biomedical optics, absorption of photons is a most important event:
· Absorption is the primary event that allows a laser or other light source to cause a potentially therapeutic (or damaging) effect on a tissue. Without absorption, there is no energy transfer to the tissue and the tissue is left unaffected by the light.
· Absorption of light provides a diagnostic role such as the spectroscopy of a tissue. Absorption can provide a clue as to the chemical composition of a tissue, and serve as a mechanism of optical contrast during imaging. Absorption is used for both spectroscopic and imaging applications.
Molecules that absorb light are called chromophores. Some examples of chromophores are water, blood (hemoglobin), melanin, amino acids and fatty acids.
In the UV: tissue absorption is high due to protein, amino acid, fatty acid and DNA absorption
In the IR: tissue absorption is dominated by water absorption
In the visible: whole blood (hemoglobin) is a strong absorber for some wavelengths (blue/green) but since the fraction of blood in tissue is small average tissue absorption is minimal unless you are looking at a blood vessel. Melanin (melanosome) is a strong absorber, again small on average except when looking at areas with strong pigmentation such as the skin.
The absorption of light can be characterized using Beer's Law by which light that goes in to a material decays exponentially.
Then:

Where: E0 is the incident irradiance
E(z) is the irradiance through some distance z of the medium
c is the concentration of the absorbing medium and
x(l) is molecular absorption coefficient (also known as the molar extinction coefficient) which is a function of the wavelength
This relationship is a standard exponential decay (known as Beer's law).
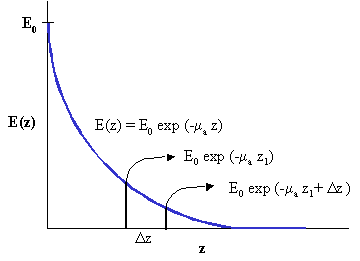
The ratio of E(z) to E0 gives the percent transmission through a layer with thickness z:
![]()
Also note that the if you plot E(z) as function of z on a log plot, this curve will be a straight line, the slope of which will be the absorption coefficient.
Oftentimes, c and x(l) are not known for tissue. Instead we lump the two together and use a probability approach. We then replace (cx(l)) with the absorption coefficient (ma). And rewrite Beer's Law as
![]()
Definition absorption coefficient: When a photon travels over an infinitesimal distance Dz the probability for absorption is given by ma Dz where ma is defined as the absorption coefficient (m-1) (i.e. 1/ma is the mean free path a photon travels before for an absorption event takes place).
Example 1: When light travels through a slab of medium, for every Dz, there is 50% absorption. Plot the attenuation of 100 photons travelling through this medium if the medium is 20 Dz thick.
For every Dz, since there is 50% absorption,
E = 0.5E0,
E / E0 = 0.5 = exp(-ua z)
Therefore,
ln(0.5) = (-ua z)
ua = 0.69 cm-1 (assuming z = 1 cm)
Shown below is the Beer's Law attenuation that can be seen for the case.

The probability that a photon is absorbed in a distance less than z1 is given by the probability
![]()
where the probability defines a probability distribution function denoted by F(z1)

The probability that a photon is absorbed between z and z + dz, divided by dz, is given by the probability density function f which is the derivative of the probability distribution function.
![]()

Penetration Depth:
At some depth we let z equal 1 / ua: z = d = 1 / ma
At that point:
![]()
Heat Source Term:
Remember that E - irradiance is power per unit area. Thus the irradiance gives us information about how much light made it to a certain point in the tissue. It does not tell us how much of that light was absorbed at that point. We define a new term called the Heat Source term S as the number of photons absorbed per unit volume in W/m3. Note that number of photons absorbed can be related to amount of heat generated i.e. heat source.
Mathematically, heat source can be written as
![]()
Example:
Historically photocoagulation of the retina has been an effective treatment of diabetic retinopathy (angiogenesis and leaky vessels). In this case the objective is to coagulate the majority of the retina in an attempt to save the fovea. Also in retinal tears, photocoagulation is effective. Here the task is to "spotweld" the retina to the underlying choroid.
Plot the irradiance and heat source for light incident on the eye.

Scattering
Scattering of light occurs in media that contains spatial fluctuations in the refractive index n, whether such fluctuations are discrete particles or more continuous variations in n.
In biomedical optics, scattering of photons is an important event:
· Scattering provides feedback during therapy. For example, during laser coagulation of tissues, the onset of scattering is an observable endpoint that signals a desired therapeutic goal. Scattering also strongly affects the dosimetry of light during therapeutic procedures that depend on absorption. The scattering affects "where" the light goes and thus where absorption will occur.
· Scattering has diagnostic value. Scattering depends on the microstructure of a tissue, e.g., the density of lipid membranes in the cells, the size of nuclei, the presence of collagen fibers, the status of hydration in the tissue, etc. Scattering is used for both spectroscopic and imaging applications.
Scattering Coefficient: When a photon travels over an infinitesimal distance Dz, the probability for scattering is given by ms Dz where ms is defined as the scattering coefficient (m-1). The mean free path of scattering is 1/ µs.
When both absorption and scattering are present, then we define the total attenuation coefficient,
![]()
Light scattered from the collimated beam undergoes multiple scattering events as it propagates through tissue. The "transport theory" is used to describe the transfer of energy through tissue. This theory is based on a statistical approximation of photon particle transport in a multiple scattering medium.

The phase function p(s, s') represents the probability that a photon will scatter from direction s into direction s'.
The light transport equation: relates the gradient of radiance at position 'r' in direction s to losses due to absorption and scattering and gain due to scattering from all other directions s' into s.

![]() - change in radiance at r in the direction s.
- change in radiance at r in the direction s.
L(r, s) - radiance defined as the propagation of photon power
![]() - losses due to absorption
- losses due to absorption
![]() - losses due to scattering
- losses due to scattering
![]() - gain due to scattering from all s' into s where p(s, s') is the phase function.
- gain due to scattering from all s' into s where p(s, s') is the phase function.
S(r, s) - source of power generated at r in the direction s (which may be due to fluorescence or due to some kind of internal light source)
Phase function: A sphere contains 4pi radians. For isotropic materials, the phase function is constant and equal to 1/4pi. In other words, there is equal probability that the photon will scatter in every direction.
Unfortunately, light scattering in tissue is not isotropic; it is strongly forward directed. A measure of the degree of anisotropy in scattering is given by the anisotropy factor, g where,
![]()
That looks complicated. An easier way to remember this is the g is the average cosine of the scattering angle, O. With this it should be easy to understand that:
Total forward scattering: g = 1
Isotropic scattering: g = 0
Total backscattering: g = -1
For in vitro tissues in the visible and near- IR wavelengths, g " 0.7-0.9.
Thus, we now not only know something about the probability that scattering will happen, we also know something about the direction in which scattering will happen. With this we can define a few new useful parameters:
Reduced scattering coefficient: µs' = µs(1 - g)
Reduced attenuation coefficient: µt = µa + µs'
Effective attenuation coefficient: µeff = sqrt [3µa (µa + µs ')]
Penetration depth = mean free path = 1/ µt
Effective penetration depth: deff = 1/ µeff
How to get or measure optical properties?
In a purely absorbing material, one can use Beer's Law to obtain the absorption coefficient. However, in order to obtain the optical properties of tissues there is no direct way to do so. In vitro, for a semi-infinite slab that is optically thick, although the optical properties cannot be directly measured and indirect approach is taken. The diffuse reflectance (R) and diffuse transmission (T) are first measured.
Diffuse reflectance: Of the light reflected off the surface, a small percent can be calculated to be reflected due to the index mismatch at the surface - this is referred to as specular reflectance. The light that is reflected off the surface after having undergone one or more scattering events is called diffuse reflectance.
To measure R and T: The most common way is by using an integrating sphere. An integrating sphere is a sphere with 2 ports and a detector (see figure) in which the inside is coated with a highly reflective material.

Once R and T are measured, the light transport equation is solved in an inverse manner to obtain the optical properties. i.e. assume initial value of ma, ms and g, calculate R and T. Keep changing ma, and ms' until measured R and T is obtained.
Different models can be used to solve the light transport equation. These include
· Adding - Doubling Method
· Delta - Eddington Method
· Diffusion Approximation Method
· Monte Carlo Method
It is however not feasible in most tissues to measure transmission in vivo. However just the measurement of reflectance if cleverly done can provide significant information about the optical properties (absorption coefficient and reduced scattering coefficient) of the tissue. Ex vivo measurements do allow transmission measurement and the optical properties obtained in this fashion can be used in dosimetry calculations.
